You're tired. Not just "I need another coffee" tired, but a deep, bone-weary fatigue that sticks with you all day. Maybe you lie awake for hours watching the clock, or your partner complains your snoring sounds like a freight train. You might brush it off as stress, aging, or just a bad patch. But when does a string of rough nights cross the line into a real sleep disorder? The answer isn't always obvious, and that's why so many people suffer for years without getting help.
I've spent over a decade researching sleep health and talking to people who've been through this. The most common mistake I see? People compare their sleep to an unrealistic ideal or dismiss their symptoms because they've gotten used to feeling terrible. They think, "Well, I'm not falling asleep at my desk, so it must be fine." Let me be clear: a sleep disorder often doesn't announce itself with dramatic collapse. It chips away at your health, mood, and cognitive function slowly, making the new abnormal feel normal.
What's in this guide?
The Major Red Flags You Can't Ignore
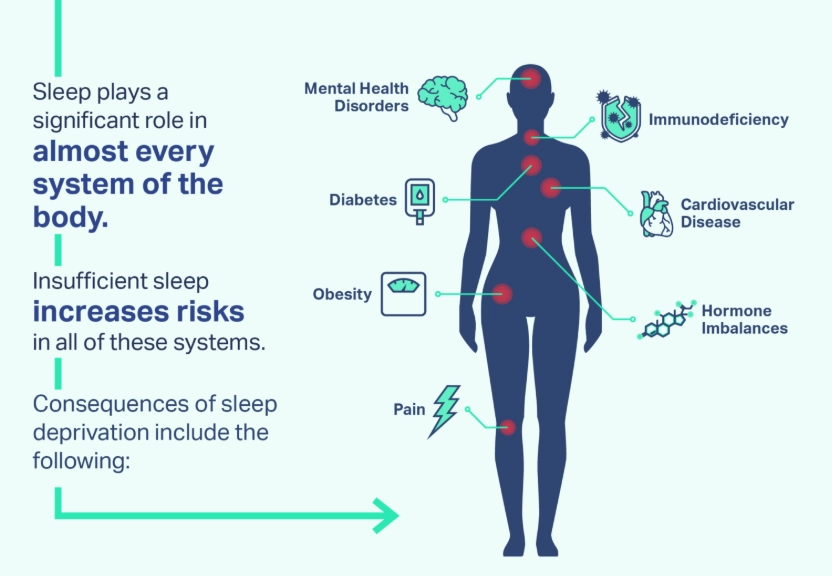
Think of these as the universal warning lights on your body's dashboard. If one or more of these persist for over three months, it's time to investigate seriously.
Your daytime function is consistently impaired. This is the core issue. It's not just about the hours in bed. Do you struggle with concentration, memory lapses ("What did I just walk into this room for?"), irritability, or low motivation most days? Is driving feel dangerously monotonous? This daytime fallout is a primary diagnostic criterion for disorders like insomnia, as outlined by the American Academy of Sleep Medicine.
You need excessive time to fall asleep or stay asleep. Lying awake for more than 30 minutes most nights trying to fall asleep, or waking up for long periods in the middle of the night, points directly toward insomnia. Waking up more than an hour before your alarm and being unable to drift back off is another classic sign.
You're told you snore loudly, gasp, or stop breathing. This is the hallmark of sleep apnea, and you often won't know it yourself. A bed partner's observation is crucial. It's not just annoying snoring; it's a sign of obstructed airways.
You have an uncontrollable urge to move your legs at night. That creepy-crawly, itchy, or aching sensation in your legs that only improves with movement is Restless Legs Syndrome (RLS). It typically strikes in the evening when you're trying to relax.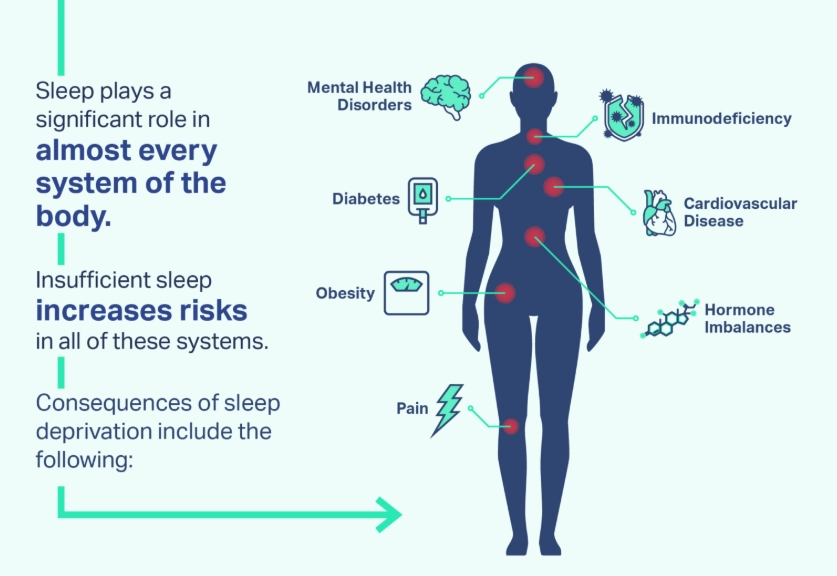
Key Insight: Many people fixate on total sleep time. "I get 6 hours, that's enough, right?" But the quality and continuity of those 6 hours matter far more. You can be in bed for 8 hours with severe sleep apnea and get zero restorative deep sleep. Focus on how you feel and function, not just the clock.
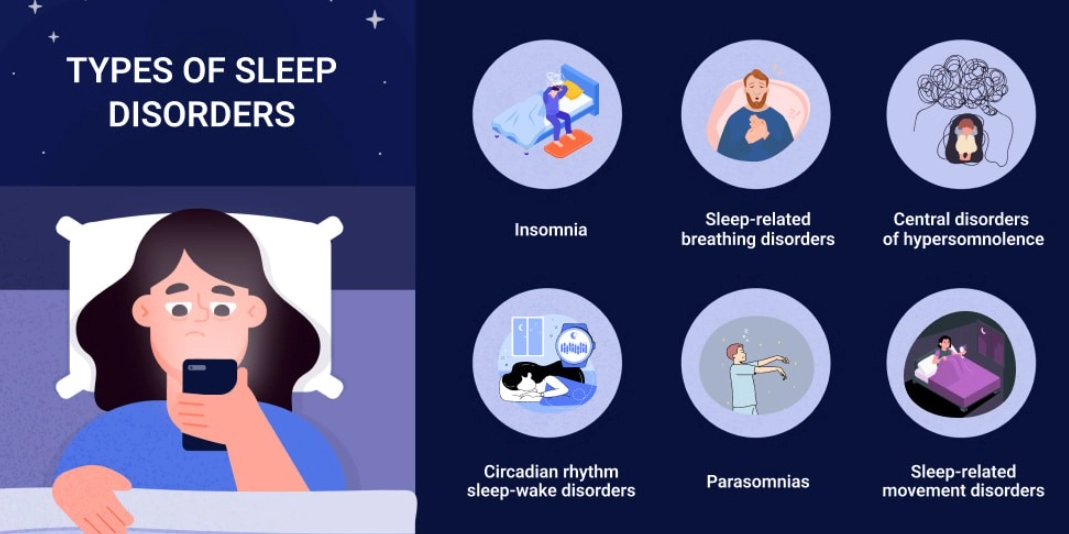
Common Sleep Disorders and Their Specific Signs
Sleep disorders have distinct fingerprints. Here’s how to tell them apart.
Insomnia: The Mind That Won't Shut Off
This isn't occasional trouble sleeping. Chronic insomnia involves a persistent difficulty initiating or maintaining sleep, despite having adequate opportunity to sleep, leading to daytime consequences. The mental component is huge. You might experience:
- Sleep anxiety: Dreading bedtime, feeling your heart race as you get into bed.
- Rumination: Your brain replaying the day's events or tomorrow's to-do list on a loop.
- Conditioned arousal: Your bed becomes associated with frustration and wakefulness, not rest.
Sleep Apnea: The Silent Nighttime Choking
In obstructive sleep apnea (OSA), your airway collapses repeatedly during sleep. Each collapse (apnea) causes a brief drop in blood oxygen and a micro-awakening to restart breathing. You might not remember these awakenings, but your body does. Signs include:
- Loud, chronic snoring punctuated by silence (the apnea), then a gasp or choke. >Waking up with a dry mouth or sore throat. >Morning headaches. >Excessive daytime sleepiness, sometimes leading to unintentional naps.
I had a friend who blamed his crushing fatigue on his job for years. He was thin and active, so he never considered sleep apnea. It was only after his wife recorded his gasping at night that he got tested and was diagnosed with a moderate case. The stereotype that it only affects overweight, older men is dangerously wrong.
Restless Legs Syndrome (RLS) & Periodic Limb Movement Disorder (PLMD)
RLS is the uncomfortable sensory urge; PLMD is the physical kicking or jerking that happens during sleep itself, often disrupting it. You might have both. A partner might complain of being kicked all night.
Circadian Rhythm Disorders
Your internal clock is misaligned with the world. In Delayed Sleep-Wake Phase Disorder, you're a true "night owl," unable to fall asleep before 2-3 AM and struggling to wake for a 7 AM job. It's not laziness; it's a biological mismatch.
| Disorder | Primary Nighttime Sign | Primary Daytime Sign | Often Mistaken For... |
|---|---|---|---|
| Insomnia | Prolonged awakening in bed, mind racing | Fatigue, brain fog, irritability | Stress or anxiety disorder |
| Sleep Apnea | Loud snoring/gasping (observed by others) | Excessive sleepiness, unrefreshing sleep | Depression, aging, or just being "a bad sleeper" |
| Restless Legs Syndrome (RLS) | Urge to move legs when resting in evening | Daytime fatigue from disrupted sleep | Nervousness, arthritis, or "just fidgety" |
| Delayed Sleep Phase | Can't sleep until very late (e.g., 3 AM) | Extreme difficulty waking early, grogginess | Poor discipline, insomnia, or laziness |
A Practical Self-Assessment: Your Sleep Health Checklist
Don't just guess. Take notes for a week or two. Track these things in a notebook or app:
- Bedtime & Lights-Out Time: When do you actually try to sleep?
- Estimated Sleep Onset: How long does it take?
- Night Wakings: How many times? For how long?
- Final Wake-Up Time: Is it before the alarm?
- Total Sleep Time (estimate):
- Day 1 Feelings: Rate your energy, mood, focus on a 1-10 scale.
- Partner Observations: Ask about snoring, gasping, or movements.

Then, ask yourself these questions honestly:
- Do I feel refreshed and alert for most of the day, or do I hit a major slump?
- Do I rely on caffeine or sugar to get through the afternoon?
- Has my mood or patience taken a noticeable hit?
- Have I dozed off unintentionally (in meetings, watching TV, or worse, while driving)?
If you're answering negatively to these, your sleep is likely failing its primary job.
What to Do Next: From Doctor Visits to Diagnosis
You've noticed the signs. Now what? Don't go straight to Dr. Google for a cure. The path is clearer than you think.
1. Start with Your Primary Care Physician (PCP). Bring your sleep log. Describe your symptoms and their daytime impact clearly. Say, "My snoring is disrupting my partner, and I'm exhausted every day despite being in bed for 8 hours," not just "I'm tired." Your PCP can rule out other issues (thyroid problems, anemia, depression) that mimic sleep disorder symptoms.
2. Expect a Referral to a Sleep Specialist. For suspected apnea, RLS, or complex insomnia, a sleep medicine doctor is the expert. They'll conduct a detailed interview about your sleep habits, medical history, and symptoms.
3. The Sleep Study (Polysomnography). This is the gold standard for diagnosing sleep apnea, PLMD, and other disorders. It's not always an overnight lab stay anymore. For many, a home sleep apnea test (HSAT) is prescribed first. It's a simplified device you use at home that tracks your breathing, oxygen levels, and effort. It's less comprehensive than a lab study but excellent for catching moderate to severe apnea.
4. Getting Your Results and a Treatment Plan. A sleep specialist will interpret the data. For apnea, treatment often starts with a CPAP machine, which keeps your airway open with gentle air pressure. For insomnia, the first-line treatment is usually Cognitive Behavioral Therapy for Insomnia (CBT-I), a structured program that addresses the thoughts and behaviors ruining your sleep. It's more effective long-term than sleeping pills.
The process might seem daunting, but it's a straight line from problem to solution. Taking that first step with your doctor is the hardest and most important part.
Your Sleep Questions, Answered
I sleep 8 hours but wake up exhausted. Could this still be a sleep disorder?
Absolutely, and this is a huge red flag for sleep apnea or poor sleep quality. You might be getting 8 hours of fragmented, light sleep with no deep or REM sleep due to constant breathing disruptions (apneas). Quantity does not equal quality. A sleep study can measure your sleep architecture to see if you're actually cycling through the necessary restorative stages.
My partner says I snore, but I feel fine. Do I really need to get checked?
You might feel "fine" because you've adapted to a state of chronic sleep deprivation and oxygen deprivation. The damage from untreated sleep apnea is insidious and cumulative, raising your risk for high blood pressure, heart disease, stroke, and type 2 diabetes. Your partner's observation is a gift—it's an early warning system for a serious health condition. Getting evaluated is a proactive health move, not just about snoring.
 I've had insomnia for years and tried everything (meditation, no screens, etc.). What am I missing?
I've had insomnia for years and tried everything (meditation, no screens, etc.). What am I missing?
You're likely missing the structured, behavioral component. Many DIY approaches are pieces of the puzzle, but chronic insomnia often requires the full protocol of CBT-I. A common mistake is spending too much time in bed "trying" to sleep, which weakens the brain's association between bed and sleep. CBT-I might temporarily restrict your time in bed to rebuild that connection—a counterintuitive step most people won't try on their own. Working with a therapist trained in CBT-I is the most effective path for long-term change.
Are over-the-counter sleep trackers (like Fitbit or Oura Ring) accurate for diagnosing a disorder?
They are useful tools for spotting trends—like consistently low sleep duration or frequent awakenings—and can provide great data for your doctor. However, they cannot diagnose a sleep disorder. Consumer devices are not medical-grade. They can't detect sleep apnea (they guess based on movement and heart rate variability) or measure brain waves to assess sleep stages accurately. Use them as a guide for conversation, not as a diagnostic device.
I'm scared of being hooked on sleeping pills if I see a doctor. Is that the only option?
Not at all, and a reputable sleep specialist will share that concern. For insomnia, CBT-I is the recommended first-line treatment because it addresses the root cause without medication. For sleep apnea, the treatment is a CPAP device, not pills. Medication might be considered for short-term use or in specific cases, but it's not the default or only solution. A good doctor will explore all options with you.
 Knowing if you have a sleep disorder starts with listening to your body and trusting that persistent fatigue, mood swings, and brain fog aren't just "part of life." They're signals. By understanding the specific signs, keeping a simple log, and taking that information to a doctor, you move from guessing to knowing. From there, effective, often life-changing treatment is not just possible—it's the most likely outcome. Your path to better sleep and better days begins with recognizing that something's off and deciding to look into it.
Knowing if you have a sleep disorder starts with listening to your body and trusting that persistent fatigue, mood swings, and brain fog aren't just "part of life." They're signals. By understanding the specific signs, keeping a simple log, and taking that information to a doctor, you move from guessing to knowing. From there, effective, often life-changing treatment is not just possible—it's the most likely outcome. Your path to better sleep and better days begins with recognizing that something's off and deciding to look into it.
Reader Comments