You're here because you're tired of being tired. Maybe you lie awake for hours, or you wake up feeling like you never slept. Perhaps your partner complains about your snoring, or you have this irresistible urge to move your legs at night. The question "what sleep disorder do I have?" is more than just curiosity—it's a search for answers to reclaim your energy, mood, and health. Let's cut through the confusion. This guide won't give you a diagnosis (only a doctor can do that), but it will help you connect your specific, frustrating symptoms to the most common sleep disorders and show you exactly what to do next.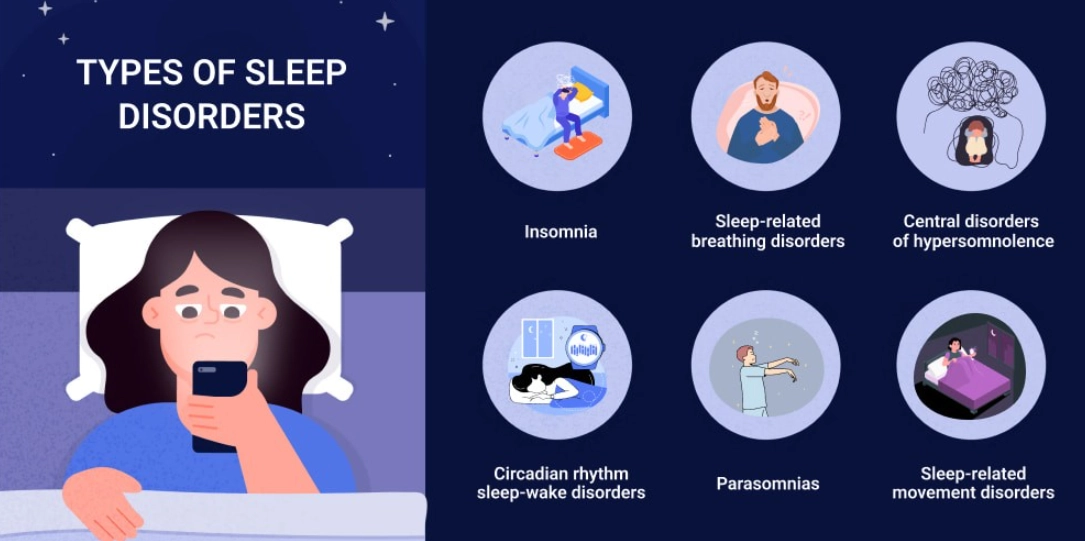
What You'll Find in This Guide
Understanding the Major Types of Sleep Disorders
Sleep issues aren't one-size-fits-all. The term "sleep disorder" covers over 80 different conditions. But most people struggling with "what sleep disorder do I have" are dealing with one of a handful of common culprits. The key is in the specific symptoms and their timing.
Here’s a breakdown of the big players. Look for the pattern that matches your nightly battle.
| Disorder | Core Symptom (The "What") | Typical Timing & Feelings | Who It Often Affects |
|---|---|---|---|
| Insomnia | Chronic difficulty falling asleep, staying asleep, or waking too early. | Lying awake with a racing mind at bedtime or in the middle of the night. Daytime fatigue, irritability, poor concentration. | Highly stressed individuals, those with anxiety/depression, shift workers. Very common. |
| Sleep Apnea (Obstructive) | Breathing repeatedly stops and starts during sleep. | Loud, chronic snoring, gasping/choking sounds at night. Waking up unrefreshed despite long hours in bed. Morning headaches. | Often linked to being overweight, having a large neck circumference, or a family history. More common in men, but underdiagnosed in women. |
| Restless Legs Syndrome (RLS) | An uncomfortable, irresistible urge to move the legs. | Worse in the evening and at rest (sitting/lying). Temporarily relieved by movement. Can severely delay sleep onset. | Can be genetic. Associated with iron deficiency, pregnancy, kidney disease. |
| Narcolepsy | Overwhelming daytime sleepiness and sudden "sleep attacks." | Falling asleep involuntarily in quiet situations (e.g., in a meeting). May include cataplexy (sudden muscle weakness with emotion). | Often begins in teens/young adults. It's a neurological disorder, not just being "really tired." |
| Circadian Rhythm Disorders | Your internal body clock is out of sync with the day-night cycle. | If you're a "night owl" (Delayed Sleep-Wake Phase): can't sleep until 2-3 AM, struggle to wake for work/school. The opposite pattern also exists. | Teens/young adults (night owls), shift workers, frequent travelers with jet lag. |
One mistake I see people make all the time is mixing up symptoms and causes. For example, anxiety can cause insomnia, but chronic insomnia then worsens anxiety—it becomes a vicious cycle. The disorder is the persistent pattern of disrupted sleep, regardless of what kicked it off initially.
Your Self-Assessment: Three Practical Steps
Before you dive down a WebMD rabbit hole, do this instead. It’s what I advise friends and family to do first.
Step 1: The Two-Week Sleep Diary
Forget trying to remember how you slept last Tuesday. Our perception is fuzzy. You need data.
Every morning, jot down these four things in a notebook or app:
- Bedtime & Lights-Out Time: When you got into bed vs. when you actually tried to sleep.
- Estimated Sleep Onset: How long it took to fall asleep.
- Night Wakings: How many times you woke up and for how long.
- Final Wake Time & Out-of-Bed Time: When you woke up for good vs. when you got up.
- Sleep Quality (1-5 scale): Your gut feeling.
- Daytime Notes: Naps, caffeine/alcohol intake, stress levels, exercise.
After two weeks, look for patterns. Do you see consistent long sleep latency (time to fall asleep)? That points toward insomnia or RLS. Do you note frequent, brief awakenings you can't explain? That could be sleep apnea. The diary removes the emotion and gives you facts to bring to a doctor.
Step 2: Involve Your Sleep Partner (If You Have One)
They are your best witness. Ask them, calmly, to tell you what they observe. Do you snore loudly and then go quiet? (A classic sign of apnea). Do you kick or thrash your legs periodically? (Could be RLS or Periodic Limb Movement Disorder). Do you seem to stop breathing? Their observations are pure gold for narrowing down "what sleep disorder do I have."
Step 3: Use a Validated Screening Tool
These are short questionnaires doctors use. Don't just Google random quizzes. Go to authoritative sources. Two of the best are:
- The Epworth Sleepiness Scale: Measures your likelihood of dozing off in daily situations. A high score (>10) suggests significant daytime sleepiness, common in sleep apnea, narcolepsy, or severe insomnia. You can find it on the American Sleep Association website.
- The STOP-BANG Questionnaire: A quick 8-question screen for Obstructive Sleep Apnea risk. It asks about Snoring, Tiredness, Observed apnea, high blood Pressure, etc. Many hospital sleep centers have it online.
When and How to Talk to a Doctor
So you've tracked your sleep and have suspicions. When is it time to get professional help?
See a doctor if your sleep problems:
- Happen three or more nights per week for over a month. >Significantly impact your
- (you're falling asleep at your desk, making errors, feeling depressed). >Affect your
- (drowsy driving is a major red flag). >Involve
- or
- .
Start with your primary care physician (PCP). Come prepared. Don't just say "I'm tired." Bring your sleep diary, your partner's observations, and your Epworth score. Say: "I've been struggling with insomnia for 8 weeks. My sleep diary shows it takes me over 90 minutes to fall asleep most nights, and I'm worried about my concentration at work." This specific, data-driven approach gets you taken seriously and fast-tracks you to the right specialist, usually a sleep medicine physician or a pulmonologist (for apnea), neurologist (for RLS, narcolepsy), or psychologist/psychiatrist (for insomnia related to mental health).
What Happens During a Professional Sleep Study?
The idea of a sleep study (polysomnogram) can be intimidating. Let's demystify it. It's the gold standard for diagnosing many sleep disorders, especially sleep apnea, narcolepsy, and periodic limb movements.
You'll go to a sleep lab (or sometimes do a home test). Technicians place sensors on your scalp, face, chest, and legs to monitor:
- Brain waves (EEG): To determine sleep stages (light, deep, REM).
- Eye movements (EOG): To detect REM sleep.
- Muscle activity (EMG): For leg movements and chin tension.
- Heart rhythm (EKG): For heart rate.
- Breathing effort & airflow: To count apneas and hypopneas.
- Blood oxygen level: To see if oxygen drops during breathing pauses.
Yes, it looks weird. No, you won't sleep "normally." But here's the insider perspective: they only need 4-5 hoursof measurable sleep data to get a diagnosis for most disorders. The goal isn't to see if you sleep perfectly in a strange bed—it's to see what your brain and body do when sleep does happen. For apnea, they often do a "split-night" study: if they detect significant apnea in the first half, they'll wake you and fit you with a CPAP machine for the second half to see if it works.
Common Treatment Paths for Different Disorders
Treatment is not just "take a pill." It's targeted to the root cause.
For Insomnia: The first-line, most effective treatment is Cognitive Behavioral Therapy for Insomnia (CBT-I). It's a structured program that changes your thoughts and behaviors around sleep. It's more effective and durable than sleep medications. The CDC and the American College of Physicians recommend it as the initial treatment. It involves sleep restriction, stimulus control, and cognitive therapy.
For Sleep Apnea: The standard is CPAP (Continuous Positive Airway Pressure). A machine delivers gentle air pressure through a mask to keep your airway open. The new machines are much quieter and more comfortable than the old stereotypes. Alternatives include oral appliances (fitted by a dentist) or, for some, surgery.
For RLS: Treatment may involve correcting underlying iron deficiency (a simple blood test can check ferritin levels). Medications that affect dopamine or other brain chemicals can be very effective.
For Narcolepsy: Treatment combines scheduled naps with stimulant medications for daytime sleepiness and other drugs to manage cataplexy if present.
For Circadian Disorders: Timed light therapy (using a bright light box in the morning for night owls) and strict sleep schedule management are core treatments. Sometimes low-dose melatonin is used at specific times to shift the internal clock.
The common thread? An accurate diagnosis from a professional is essential to get on the right path. Guessing and trying over-the-counter remedies for the wrong disorder wastes time and money.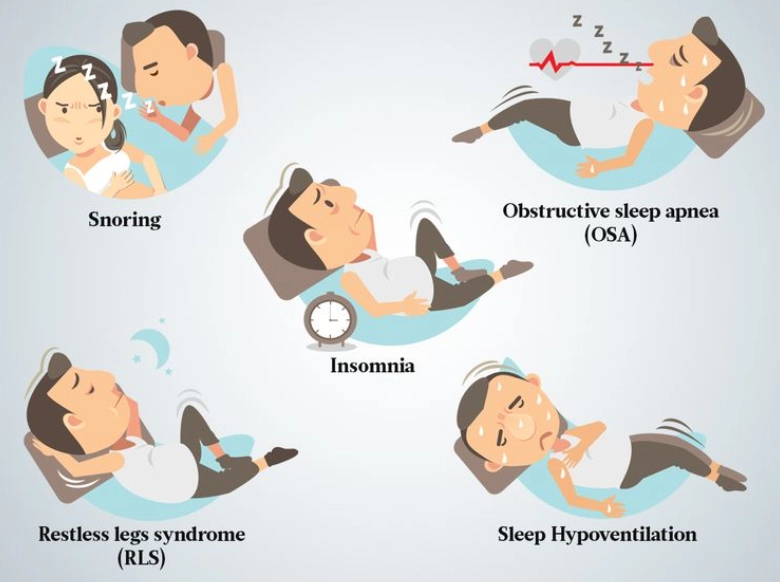
Your Questions, Answered
 Figuring out "what sleep disorder do I have" is a process. It starts with paying close attention to your own body, gathering evidence, and then partnering with a healthcare professional. The goal isn't just a label—it's a path to treatment and finally getting the rest you need. Don't resign yourself to being tired. Take that first step and track your sleep tonight.
Figuring out "what sleep disorder do I have" is a process. It starts with paying close attention to your own body, gathering evidence, and then partnering with a healthcare professional. The goal isn't just a label—it's a path to treatment and finally getting the rest you need. Don't resign yourself to being tired. Take that first step and track your sleep tonight.
Reader Comments