Quick Navigation
- The Two Main Camps: Subjective vs. Objective Measurement
- How is Sleep Quality Measured Subjectively? The Power of Your Own Perception
- How is Sleep Quality Measured Objectively? The World of Gadgets and Wires
- Key Metrics: What to Look For When You Measure Sleep Quality
- Putting It All Together: A Practical Guide to Measuring Your Own Sleep
- Common Questions About How Sleep Quality is Measured
- Final Thoughts: It's About Insight, Not Obsession
Let's be honest, we've all been there. You wake up feeling groggy, drag yourself through the day, and wonder, "Did I even sleep last night?" Or maybe you clocked a solid eight hours on your fancy smartwatch, but you still feel like you've been hit by a truck. That's when the question really hits home: how is sleep quality measured, and more importantly, which method should I trust?
I remember staring at my sleep tracker data, feeling more confused than enlightened. It said I had "good" sleep with 92% efficiency. My body begged to differ. That's when I went down the rabbit hole, talking to sleep specialists, digging into research papers, and testing every method under the moon (pun intended). What I found was a world of difference between feeling rested and what the gadgets report.
The truth is, measuring sleep quality isn't a one-size-fits-all game. It's a mix of old-school pen-and-paper methods and high-tech lab gear, each telling a different part of the story. Some methods ask you how you feel (subjective), while others try to measure what your body is actually doing (objective). Neither is perfect on its own, and that's the first big lesson.
So, if you're tired of guessing, let's break it all down. No jargon, no sales pitches, just a clear look at the tools and techniques scientists and doctors use to answer that fundamental question: how is sleep quality measured?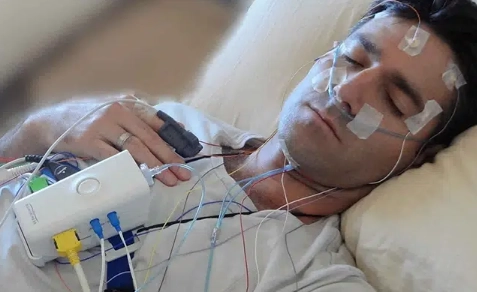
The Two Main Camps: Subjective vs. Objective Measurement
Before we dive into the specifics, it's crucial to understand this core split. The entire field of sleep assessment sits between these two pillars.
Subjective Measurement is all about your experience. How do you feel you slept? This might seem less scientific, but your perception is king when it comes to daytime function. If you feel terrible, it doesn't matter if a machine says you slept perfectly. These tools are cheap, easy, and capture the outcome that matters most—your personal restoration.
Objective Measurement tries to get at the biological truth. It uses devices to monitor bodily signals like brain waves, eye movement, heart rate, and movement. The goal is to remove human bias and see what's happening under the hood. But here's the catch: these devices can sometimes miss the forest for the trees, giving you great data about a terrible night's sleep.
The smartest approach, used in proper sleep clinics, is to combine both. They'll hook you up to machines and ask you a bunch of questions in the morning. That combination gives the full picture.
How is Sleep Quality Measured Subjectively? The Power of Your Own Perception
This is where most of us start, even if we don't realize it. Rolling over and groaning "five more minutes" is a subjective assessment. But to get useful data, we need a bit more structure.
The Humble Sleep Diary (or Sleep Log)
Don't let its simplicity fool you. The sleep diary is the gold standard for subjective measurement in clinical settings. It's literally a daily log where you jot down key details. The American Academy of Sleep Medicine (AASM) even provides standard templates because it's so valuable.
You typically record things right before bed and right after waking:
- What time you got into bed.
- How long it took to fall asleep (sleep latency).
- How many times you woke up during the night.
- Total time spent awake after initially falling asleep.
- What time you finally got out of bed for the day.
- Your estimated total sleep time.
- A simple rating of how you feel (e.g., 1-5 scale).
Doing this for just one or two weeks can reveal patterns you'd never spot otherwise. Maybe you're going to bed too late on weekends, or that afternoon coffee is causing more trouble than you thought. The act of writing it down makes it real.
Standardized Sleep Questionnaires
If a diary is a daily journal, questionnaires are the snapshot exams. They ask a set of standardized questions designed to screen for specific sleep issues or gauge overall sleep health. They're fantastic for getting a quick, comparable score. Here are the big ones:
| Questionnaire Name | What It Measures | Best For | My Take |
|---|---|---|---|
| Pittsburgh Sleep Quality Index (PSQI) | Overall sleep quality and disturbances over a one-month period. It's the most widely used research tool. | Getting a global "sleep health" score. It covers seven components like latency, duration, efficiency, and daytime dysfunction. | Comprehensive, but a bit long. The one-month recall can be tricky if your sleep is variable. |
| Insomnia Severity Index (ISI) | Exactly what it sounds like—the severity of insomnia symptoms. | Figuring out if your sleep troubles cross the line into clinical insomnia. | Short, sweet, and very focused. Great for tracking progress if you're working on insomnia. |
| Epworth Sleepiness Scale (ESS) | Your likelihood of dozing off in everyday situations (like sitting in a meeting or as a passenger in a car). | Measuring daytime sleepiness, which is a major consequence of poor sleep quality. | Simple and reveals a lot. A high score here is a major red flag to see a doctor. |
You can find these questionnaires online (the National Sleep Foundation often has them). Filling one out takes 5-10 minutes and gives you a benchmark. It's a fantastic first step before you spend money on gadgets.
But are these questionnaires reliable? Mostly, yes. They've been validated in thousands of studies. But they're still just your opinion on paper.
How is Sleep Quality Measured Objectively? The World of Gadgets and Wires
This is the flashy part. Wearables, rings, bedside devices—they all promise to give you the hard truth about your sleep. But they work in very different ways, with varying levels of accuracy.
Consumer Wearables (Smartwatches, Fitness Rings)
Your Apple Watch, Fitbit, Oura Ring, or Whoop strap. They're everywhere. But how do they actually work? Most use a combination of actigraphy and photoplethysmography (PPG).
Actigraphy is fancy talk for measuring movement. A tiny accelerometer detects when you're still (probably asleep) and when you're moving (probably awake). It's good at guessing when you're asleep vs. awake but terrible at figuring out what stage of sleep you're in.
PPG is that green light on the back of your watch. It shines light into your skin and measures how it bounces back to detect blood volume changes. From this, the device estimates your heart rate and heart rate variability (HRV). The algorithm then makes an educated guess: dropping heart rate + low HRV + no movement = likely deep sleep. Increased HRV + some movement = likely REM sleep.
I've worn three different devices at once, and the results were laughably different. One said I got 45 minutes of deep sleep, another said 72, a third said 110. Which one was right? Probably none of them perfectly. But they all agreed I slept terribly after that late-night pizza, so the trend was clear.
The Gold Standard: Polysomnography (PSG)
If you want to know how is sleep quality measured in the most accurate way possible, this is it. Polysomnography is the overnight sleep study you do in a lab or sometimes at home. It's what doctors use to diagnose sleep disorders like apnea, narcolepsy, or periodic limb movement disorder.
They hook you up to a bunch of sensors that measure:
- Electroencephalography (EEG): Brain waves. This is the only way to definitively know what sleep stage you're in (N1, N2, N3, REM).
- Electrooculography (EOG): Eye movements. Crucial for identifying REM sleep, where your eyes dart around.
- Electromyography (EMG): Muscle tone, usually on the chin and legs. Muscles are mostly paralyzed during REM sleep.
- Respiratory Effort & Airflow: To detect pauses in breathing (apneas).
- Pulse Oximetry: Blood oxygen levels.
- Electrocardiography (ECG): Heart rhythm.
A trained sleep technologist watches the data live from another room. In the morning, a sleep physician scores the entire night in 30-second chunks, following strict rules from the AASM. The result is a monstrously detailed report called a hypnogram.
Obviously, you don't need this for general curiosity. It's expensive, inconvenient, and you'll likely sleep worse in a strange lab. But for diagnosing serious problems, it's unbeatable. The National Heart, Lung, and Blood Institute (NHLBI) has great resources on when a sleep study is medically necessary.
Other Objective Methods You Might Encounter
At-Home Sleep Apnea Tests (HSAT): These are simplified devices you use at home, usually just for screening obstructive sleep apnea. They measure airflow, breathing effort, heart rate, and oxygen levels, but NOT brain waves. So they can't measure sleep stages. They answer a specific question: "Do I have apnea?" not "What is my sleep architecture?"
Actigraphy Watches (Medical Grade): These look like a chunky plastic watch. They're prescribed by doctors for longer-term monitoring (e.g., over two weeks). They use highly calibrated movement sensors and sophisticated algorithms, often outperforming consumer wearables. They're great for diagnosing circadian rhythm disorders.
Key Metrics: What to Look For When You Measure Sleep Quality
Alright, you've got data. Now what does it all mean? When you're trying to figure out how is sleep quality measured, these are the numbers that matter most, whether they come from a diary or a device.
The Big Four Metrics
- Sleep Latency: How long it takes you to fall asleep. The sweet spot is between 10 and 20 minutes. Falling asleep in under 5 minutes might signal severe sleep deprivation. Taking over 30 minutes regularly could point to insomnia.
- Sleep Efficiency: This is a killer metric. It's the percentage of time you were actually asleep while in bed. Formula: (Total Sleep Time / Time in Bed) x 100. Anything above 85% is generally considered good. Below 75% is a problem. It captures both trouble falling asleep and trouble staying asleep.
- Wake After Sleep Onset (WASO): The total time you spend awake after initially falling asleep. A little is normal, but more than 20-30 minutes total per night can be disruptive. This is where sleep trackers and diaries often disagree—trackers might miss brief awakenings you remember, or detect micro-awakenings you don't.
- Sleep Stages (Cycle): The proportion of Light, Deep, and REM sleep. A healthy adult typically gets about 50% Light, 20-25% Deep, and 20-25% REM. The real magic is in the cycle—going through a full Light-Deep-REM sequence every 90-120 minutes. Disrupted cycles are a hallmark of poor sleep quality.
But here's a personal opinion: people get way too obsessed with sleep stages from their wearables. The absolute numbers are probably wrong. Instead, look for changes. Did your deep sleep drop suddenly for three nights in a row? That's a signal worth investigating (stress? illness? new medication?).
The Forgotten Metric: How You Feel
Never let the data overrule your own senses. Create your own morning score. On a scale of 1-10, how refreshed do you feel? How is your mood? Your energy? Your ability to focus? Log this next to your gadget's score for a week. You might find a correlation, or you might find that the gadget's "80" score feels like a "3" to you. That disconnect is valuable information.
Your body's report card is the one that matters for your day.
Putting It All Together: A Practical Guide to Measuring Your Own Sleep
So, you want to get serious about understanding your sleep. Where do you start without getting overwhelmed?
Step 1: The Two-Week Diary Baseline. Before you spend a dime, do this. Use the AASM template or just a notebook. It's free and will give you profound insights into your habits and perceptions. This is your subjective baseline.
Step 2: Add a Wearable for Trends. Pick one device you're comfortable with (watch, ring, under-mattress pad). Wear it consistently for at least a month. Ignore the absolute numbers on any given night. Instead, look at the weekly averages and trends. Is your sleep efficiency trending up or down? Is your resting heart rate during sleep creeping higher (a sign of stress or poor recovery)?
Step 3: Correlate & Investigate. This is the fun detective work. When your diary says you felt awful, what did the wearable say? Maybe it showed high WASO. When you felt great, did you notice you went to bed an hour earlier? Look for patterns between your lifestyle (caffeine, alcohol, exercise, stress), your subjective feelings, and the objective data.
Step 4: Know When to See a Professional. If your diary and tracker consistently show poor sleep (efficiency consistently below 75%, high Epworth Sleepiness Scale score, frequent long awakenings) and it's affecting your life, talk to your doctor. They might recommend an actigraphy study or a polysomnogram. Don't use a consumer device to self-diagnose sleep apnea or other disorders.
Common Questions About How Sleep Quality is Measured
Final Thoughts: It's About Insight, Not Obsession
Learning how is sleep quality measured can be enlightening, but it can also lead to a weird anxiety called "orthosomnia" – an unhealthy preoccupation with perfect sleep data. I've been there, checking my sleep score before I even said good morning to my partner. It's counterproductive.
The goal of measuring sleep isn't to get a perfect score every night. That's impossible. The goal is to gain insights that help you make small, sustainable changes. Maybe you learn that alcohol, even just one drink, ruins your sleep architecture. Maybe you see that a consistent bedtime is the single biggest factor in how you feel.
Use the tools as guides, not judges. Let the data inform you, not define you. Start simple, be consistent, and always, always listen to your own tired (or hopefully, rested) body. It's the most sophisticated measuring device you'll ever own.
Because at the end of the day, the best answer to "how is sleep quality measured?" might just be: by how you live your waking hours.
Reader Comments