You're not alone if you're lying awake at night wondering how to treat a sleeping disorder. That feeling of exhaustion mixed with frustration is all too common. Maybe you've tried counting sheep, drinking warm milk, or scrolling through endless advice online. The problem is, most advice treats sleep like a simple on/off switch, when it's more like a complex ecosystem. I've spent years researching this, and I can tell you the biggest mistake people make is treating the symptom (not sleeping) instead of the root cause (why you're not sleeping). True treatment isn't about one magic trick; it's a multi-layered approach that combines science-backed therapy, lifestyle tweaks, and sometimes medical help. Let's cut through the noise and get into what actually works.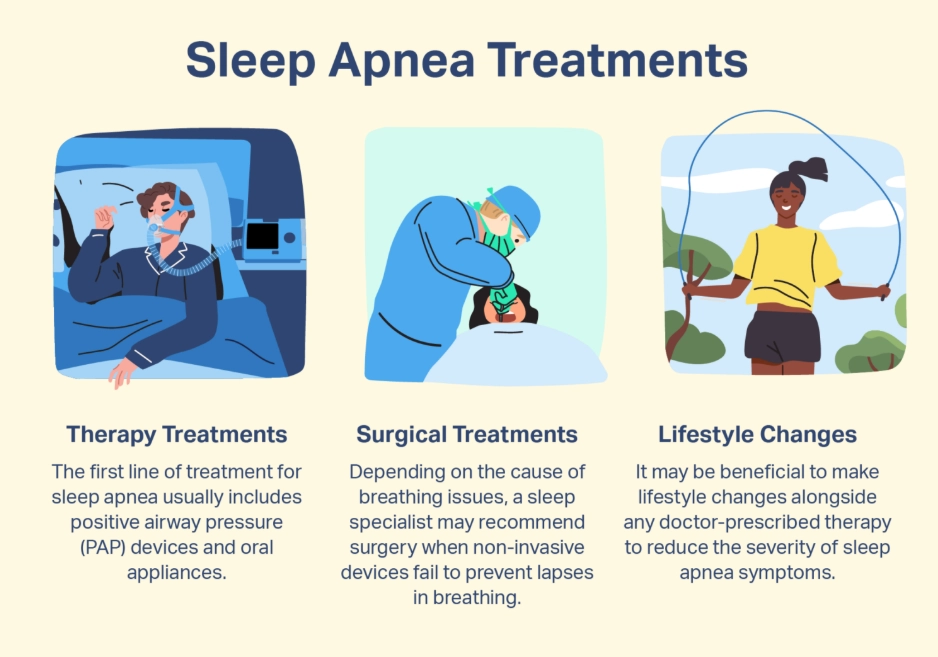
What's Inside This Guide
Understanding What a "Sleeping Disorder" Really Means
First, let's clarify the term. "Sleeping disorder" is a broad umbrella. It covers everything from chronic insomnia (trouble falling or staying asleep) to sleep apnea (breathing interruptions), restless legs syndrome, and circadian rhythm disorders. The treatment for sleep apnea (often involving a CPAP machine) is wildly different from treating insomnia. So, step one is identifying which problem you're dealing with. Many people self-diagnose with "insomnia" when their fatigue is actually due to poor sleep quality from undiagnosed apnea. That's a crucial distinction.
Think of it this way: you wouldn't treat a broken leg with cough syrup. Similarly, effective sleep disorder treatment starts with knowing the enemy.
The Critical First Step: Assessment and Diagnosis
Before jumping into treatments, you need a baseline. This isn't just about counting hours. It's about patterns. I recommend keeping a simple sleep diary for two weeks. Jot down:
- What time you got into bed.
- How long it took to fall asleep (your sleep latency).
- How many times you woke up.
- Your final wake-up time.
- Your subjective sleep quality (1-10 scale).
- Notes on caffeine, alcohol, stress, and evening activities.
This log is gold. It moves you from "I sleep terribly" to "I take 90 minutes to fall asleep on nights I work late and drink wine." That specificity is the foundation of real treatment.
Expert Insight: A common but rarely mentioned mistake is focusing solely on total sleep time. Quality trumps quantity. Six hours of solid, deep sleep can be more restorative than eight hours of fragmented, light sleep. Your diary should track how you slept, not just how long.
Core Treatment Options That Actually Work
Here’s where we get practical. Treatments fall into a few key categories. The best approach often combines them.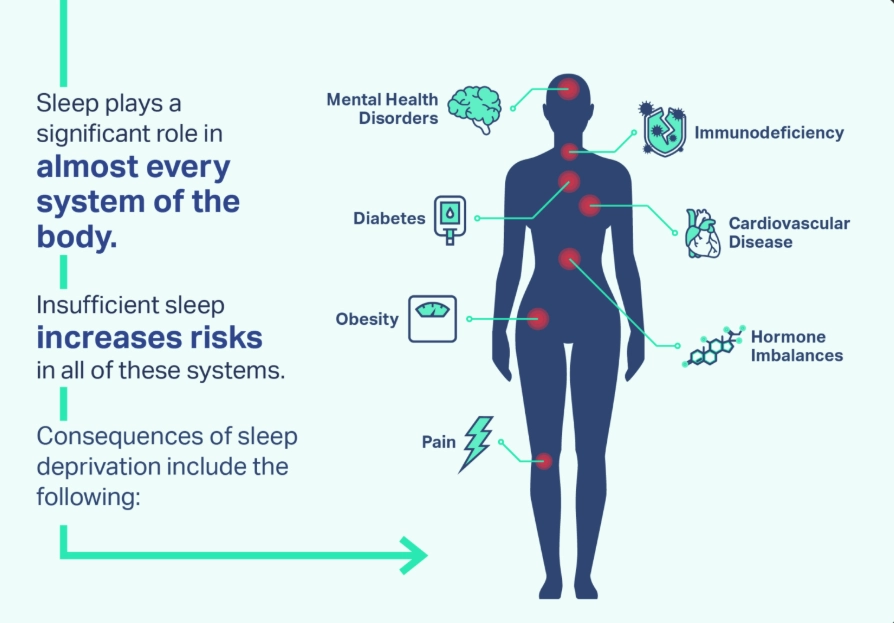
1. Cognitive Behavioral Therapy for Insomnia (CBT-I)
This is the gold-standard, first-line treatment for chronic insomnia, recommended by organizations like the American College of Physicians. It's not just talk therapy; it's a structured program that targets the thoughts and behaviors ruining your sleep.
Key Components of CBT-I:
- Sleep Restriction: Sounds counterintuitive, but it works. You temporarily limit your time in bed to match your actual sleep time. This builds sleep pressure and consolidates sleep, making it deeper and more efficient. It's the single most effective technique I've seen, but it requires guidance to do safely.
- Stimulus Control: This re-associates your bed with sleep (and sex) only. No more working, watching TV, or worrying in bed. If you're awake for 20+ minutes, you get up and do something boring in dim light until you feel sleepy again.
- Cognitive Restructuring: This challenges the catastrophic thoughts about sleep ("I'll be a wreck tomorrow!") that create anxiety and perpetuate insomnia.
You can find certified CBT-I therapists through the Society of Behavioral Sleep Medicine website. There are also reputable digital programs like Sleepio or SHUTi.
2. Medication: A Tool, Not a Solution
Sleeping pills (like zolpidem or eszopiclone) and other sedatives have their place, often for short-term use during a crisis. The problem is dependency and tolerance. They don't teach you how to sleep; they knock you out. A more nuanced approach some doctors use is low-dose antidepressants (like trazodone or doxepin) for sleep, which can be less habit-forming for some people. Melatonin supplements can help with circadian rhythm issues, like jet lag or delayed sleep phase disorder, but the dose matters—often 0.5mg to 3mg is more effective than the 10mg pills sold everywhere.
3. Treating Underlying Medical Conditions
This is non-negotiable. If you have sleep apnea, you need a sleep study and likely a CPAP device. Treating my patient's mild sleep apnea with a dental appliance was what finally cured his "insomnia." If you have restless legs, iron deficiency might be the culprit. Thyroid issues, chronic pain, and acid reflux can all destroy sleep. A full medical check-up is a critical piece of the puzzle.
| Treatment Approach | Best For | Key Consideration | Time to See Effects |
|---|---|---|---|
| CBT-I | Chronic insomnia, sleep anxiety | Requires active participation and effort | 4-8 weeks for significant improvement |
| Prescription Sleep Aids | Short-term relief, acute stress events | Risk of dependency, side effects like next-day grogginess | Immediate, but effects may diminish |
| CPAP Therapy | Obstructive Sleep Apnea | Requires adaptation to wearing a mask, but is life-changing | Often immediate improvement in sleep quality and daytime fatigue |
| Lifestyle & Sleep Hygiene | Mild sleep issues, maintenance after other treatments | Foundation for all other treatments; necessary but often insufficient alone | Consistent practice over several weeks |
Essential Lifestyle Adjustments for Lasting Change
You can't out-therapy a terrible lifestyle. These are the daily habits that support all other treatments. Think of them as the soil in which good sleep grows.
Light Exposure: This is arguably the most powerful free tool you have. Get bright, natural light in your eyes within an hour of waking. This sets your circadian clock. Conversely, dim the lights and avoid blue light from screens 2-3 hours before bed. I use amber-tinted glasses in the evening, and it made a bigger difference than any app.
The Wind-Down Routine: Your brain needs a ramp, not a cliff. Create a 60-minute buffer zone before bed. This isn't just about being "relaxed." It's about doing something genuinely enjoyable and low-stimulation: reading a physical book (not a thriller!), listening to calm music, gentle stretching, or a warm shower (the drop in body temperature afterwards promotes sleepiness).
Diet and Exercise: Regular exercise is a potent sleep aid, but timing matters. Finish vigorous workouts at least 3 hours before bedtime. Avoid heavy meals, caffeine (after 2 PM for many), and alcohol close to bed. Alcohol might make you pass out, but it fragments the second half of your sleep, making it non-restorative.
Optimize Your Sleep Environment: Cool (around 65°F or 18°C), dark, and quiet. Blackout curtains are a great investment. A white noise machine can mask disruptive sounds. Your mattress and pillows should be comfortable and supportive.
When and How to Get Professional Help
If you've tried consistent lifestyle changes for a month with no improvement, or if your sleep problem is severely impacting your mood, work, or safety (like falling asleep while driving), it's time to see a pro.
Start with your primary care physician to rule out medical issues. They can refer you to a sleep specialist (often a pulmonologist, neurologist, or psychiatrist with additional training). For insomnia-focused therapy, seek a psychologist or therapist trained in CBT-I. A sleep center can conduct an overnight polysomnography test to diagnose sleep apnea or other disorders.
Be prepared. Bring your sleep diary. Describe your problem specifically: "I have trouble falling asleep four nights a week, and it takes me over an hour" is more helpful than "I can't sleep."
Your Sleep Treatment Questions Answered
 I wake up at 3 AM every night with my mind racing. Is this a specific disorder, and how do I treat it?
I wake up at 3 AM every night with my mind racing. Is this a specific disorder, and how do I treat it? The path to treating a sleeping disorder isn't a straight line. It involves honest assessment, often a combination of behavioral therapy and lifestyle change, and sometimes professional guidance. Forget the quest for a perfect night's sleep every night. Aim for consistency and gradual improvement. Start with one thing from this guide—maybe the sleep diary or fixing your light exposure. Build from there. Your sleep is a skill you can relearn.
The path to treating a sleeping disorder isn't a straight line. It involves honest assessment, often a combination of behavioral therapy and lifestyle change, and sometimes professional guidance. Forget the quest for a perfect night's sleep every night. Aim for consistency and gradual improvement. Start with one thing from this guide—maybe the sleep diary or fixing your light exposure. Build from there. Your sleep is a skill you can relearn.
Reader Comments