We've all had a bad night. Tossing, turning, watching the clock. But when those nights string together into weeks, and fatigue becomes your default setting, it's more than bad luck—you might be facing one of the five primary categories of clinical sleep disorders. Understanding the difference between them is the first, crucial step toward fixing the problem. It's not just about being tired; disorders like sleep apnea can strain your heart, while chronic insomnia rewires your brain's stress response.
Let's cut through the noise. Here are the five main types of sleep problems that sleep medicine specialists diagnose and treat: Insomnia, Sleep Apnea, Restless Legs Syndrome, Narcolepsy, and Circadian Rhythm Disorders.
Quick Navigation: What's Keeping You Up?
#1: Insomnia – The Unwanted Awake
This is the one most people think of. But insomnia isn't just "I can't sleep." Medically, it's defined as persistent difficulty with sleep initiation, duration, consolidation, or quality that occurs despite adequate opportunity for sleep and results in some form of daytime impairment. The American Academy of Sleep Medicine provides detailed diagnostic criteria that go far beyond a simple bad night.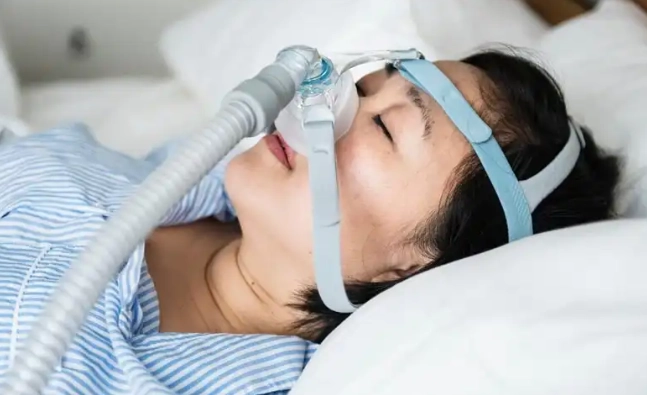
There are two main flavors:
Short-Term (Acute) Insomnia
Lasts from a few nights up to three months. It's usually tied to a clear stressor: a job interview, a fight, an upcoming deadline. Your brain is in overdrive. This is common and often resolves when the stressor passes.
Chronic Insomnia
This is the beast. It happens at least three nights a week for three months or more. Here's the subtle trap many fall into: the original stressor is gone, but you've now learned to associate your bed with anxiety and wakefulness. You start dreading bedtime, developing "sleep effort"—trying too hard to sleep, which has the opposite effect. The bed is no longer a cue for sleep; it's a cue for worry.
The gold-standard treatment isn't a pill. It's Cognitive Behavioral Therapy for Insomnia (CBT-I). A therapist helps you untangle the thoughts and behaviors fueling your insomnia. It involves sleep restriction (temporarily limiting time in bed to increase sleep drive), stimulus control (rebuilding the bed-sleep connection), and challenging catastrophic thoughts about sleep loss.
#2: Sleep Apnea – The Silent Break
If insomnia is about the brain refusing to sleep, sleep apnea is about the body being unable to breathe properly while asleep. It's far more dangerous than most people realize, linked to high blood pressure, heart disease, stroke, and type 2 diabetes.
The most common form is Obstructive Sleep Apnea (OSA). The muscles in the back of your throat relax too much during sleep, collapsing the airway. You stop breathing. Your brain gets an emergency alert, jolting you just enough to gasp and reopen the airway. This cycle can repeat hundreds of times a night, destroying sleep architecture without you ever fully waking up to remember it.
You might not be the one to notice it. A partner hears loud snoring, followed by silence (the apnea), then a choking or snorting sound. Other signs include waking with a dry mouth or headache, and that crushing fatigue no amount of coffee fixes.
Diagnosis requires a sleep study (polysomnography), either in a lab or at home with a simplified device. The primary treatment is a CPAP (Continuous Positive Airway Pressure) machine. It delivers a gentle stream of air through a mask to keep your airway open. It's not glamorous, but it's life-changing—and sometimes life-saving—for those who stick with it. Alternatives include oral appliances or, in some cases, surgery.
#3: Restless Legs Syndrome – The Nighttime Urge
RLS is a sensorimotor disorder. That's a fancy way of saying it involves strange sensations and an irresistible movement impulse. People describe it as creeping, crawling, pulling, itching, or throbbing deep inside the legs (sometimes arms). The only thing that provides temporary relief is moving.
The cruel twist? Symptoms worsen or are exclusively present during periods of rest or inactivity, especially in the evening and night. Sitting through a movie, a long flight, or trying to fall asleep becomes a battle.
A common and closely related issue is Periodic Limb Movement Disorder (PLMD), where the legs or arms jerk or twitch involuntarily during sleep every 20-40 seconds. You might not know you have it, but it fragments your sleep, leading to non-restorative sleep and daytime sleepiness.
RLS can be primary (often familial) or secondary, caused by iron deficiency, kidney disease, or pregnancy. The first step in managing it is a blood test to check ferritin (iron storage) levels. Increasing iron intake can help if levels are low. Medications like dopamine agonists or gabapentin can be prescribed for more severe cases.
#4: Narcolepsy – The Sleep Attack
Narcolepsy is often misunderstood as just "falling asleep randomly." It's a chronic neurological disorder where the brain loses its ability to regulate sleep-wake cycles normally. Think of it as a faulty light switch between wakefulness and REM (dream) sleep.
It has a classic tetrad of symptoms, though not everyone has all four:
Excessive Daytime Sleepiness (EDS): The cornerstone. A persistent, overwhelming sleepiness regardless of how much sleep you got at night. It feels like a mental fog or a constant struggle to stay awake.
Cataplexy: This is the signature symptom of Type 1 Narcolepsy. A sudden, brief loss of muscle tone triggered by strong emotions—laughter, surprise, anger. It can range from slight knee buckling to complete collapse. You remain conscious throughout.
Sleep Paralysis: Waking up unable to move or speak for a few seconds or minutes. It's terrifying but harmless.
Hypnagogic/Hypnopompic Hallucinations: Vivid, dream-like experiences when falling asleep or waking up. They feel intensely real.
Diagnosis involves a sleep study followed by a Multiple Sleep Latency Test (MSLT)—a series of daytime naps to measure how quickly you fall into REM sleep. Treatment focuses on managing symptoms with stimulants for EDS and specific medications for cataplexy. Strict sleep schedules and strategic naps are also key.
#5: Circadian Rhythm Disorders – The Misaligned Clock
Your body has a master clock in the brain (the suprachiasmatic nucleus) that runs on a roughly 24-hour cycle, dictating when you feel sleepy and alert. Circadian rhythm disorders happen when this internal clock is out of sync with your external environment (the 24-hour day).
This isn't just "I'm a night owl." It's a persistent, disabling mismatch. Two common types are:
Delayed Sleep-Wake Phase Disorder (DSWPD): Your natural sleep time is significantly later than conventional times. You can't fall asleep before 2-3 AM, and waking at 7 AM for work/school is agony. If left to your own schedule (on weekends/vacation), you sleep normally and feel fine. It's common in adolescents and young adults.
Advanced Sleep-Wake Phase Disorder (ASWPD): The opposite. You get overwhelmingly sleepy early in the evening (7-9 PM) and wake up in the very early morning (2-4 AM) unable to return to sleep. This is more common in older adults.
Shift Work Disorder and Jet Lag are also circadian rhythm problems. Treatment involves chronotherapy—strategically using light (bright light therapy lamps) and darkness, melatonin supplements, and gradually shifting sleep schedules to retrain the internal clock.
Your Sleep Questions Answered

Reader Comments