You know the feeling. It's more than just needing an extra coffee. It's a deep, bone-aching exhaustion that doesn't improve with sleep. You drag yourself through the day, your brain feels foggy, and simple tasks feel monumental. If this sounds familiar, you're not just "run down"—you might be experiencing the primary symptom of a significant underlying health issue. Extreme, persistent fatigue is the body's universal alarm bell, and for many illnesses, it's the first and loudest one to go off.
I've spent over a decade in health writing, and the most common mistake I see is people dismissing this level of fatigue for years, attributing it to stress or aging. But here's the non-consensus view: the quality of the fatigue often matters more than its severity. The fatigue of anemia feels different from the fatigue of depression, which is worlds apart from the post-exertional malaise of conditions like ME/CFS. Learning to describe it precisely is your first step toward an accurate diagnosis.
Quick Navigation: What You'll Find Here
Is It Just Tiredness, or a Medical Red Flag?
Let's clear this up first. Normal tiredness is predictable. It follows a long day, a poor night's sleep, or intense exercise. It resolves with rest. Medical fatigue is a different beast.
Medical fatigue is persistent (lasting more than two weeks), often disproportionate to your activity level, and isn't reliably relieved by sleep. It frequently comes with companions: brain fog, muscle aches, sore throat, or a general feeling of being unwell. You might hear doctors call this "asthenia" or "lethargy."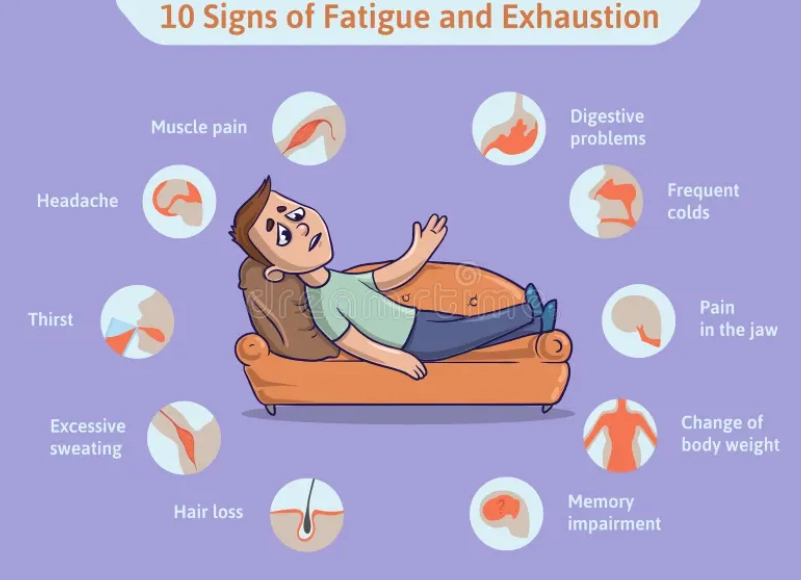
Think of it this way: If you're tired, you don't want to do the laundry. If you have medical fatigue, you want to do the laundry, but your body feels like it physically cannot. That lack of mental motivation versus physical incapacity is a key, subtle distinction.
The Top 10 Illnesses Where Extreme Fatigue Is a Hallmark Symptom
This isn't an exhaustive list, but these are the conditions where fatigue isn't just a side effect—it's frequently the presenting symptom that brings someone to the doctor. I've ordered them not by prevalence, but by how classically they manifest with debilitating exhaustion at the outset.
| Illness/Condition | Why Fatigue Happens | Other Key Early Symptoms (Besides Fatigue) |
|---|---|---|
| 1. Hypothyroidism (Underactive Thyroid) | Your thyroid gland controls metabolism. When it's sluggish, every cell in your body slows down, sapping energy. | Unexplained weight gain, feeling cold all the time, dry skin, hair loss, constipation. |
| 2. Iron-Deficiency Anemia | Low iron means your red blood cells can't carry enough oxygen to your tissues. Your body is literally running on empty. | Pale skin, shortness of breath with minimal exertion, dizziness, brittle nails, cravings for ice or dirt (pica). |
| 3. Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) | The defining feature is Post-Exertional Malaise (PEM), a crash in energy 24-48 hours after minor physical or mental effort. | Unrefreshing sleep, cognitive issues ("brain fog"), muscle/joint pain, sore throat, tender lymph nodes. |
| 4. Autoimmune Diseases (e.g., Lupus, Rheumatoid Arthritis) | The immune system attacks the body, causing widespread inflammation, which is incredibly energy-intensive. | Joint pain and swelling, low-grade fever, skin rashes (like the malar "butterfly" rash in lupus). |
| 5. Clinical Depression & Major Anxiety Disorders | Mental health conditions profoundly affect neurochemistry and stress hormones (like cortisol), draining physical energy. | Persistent sadness or worry, loss of interest in activities, changes in appetite/sleep, irritability. |
| 6. Sleep Apnea | Breathing repeatedly stops and starts during sleep, preventing deep, restorative sleep cycles night after night. | Loud snoring, gasping for air during sleep, morning headaches, daytime sleepiness, poor concentration. |
| 7. Diabetes (Type 2 & Uncontrolled Type 1) | Glucose, the body's fuel, can't get into cells efficiently. High blood sugar also causes inflammation and dehydration. | Increased thirst and urination, blurred vision, slow-healing cuts, numbness/tingling in hands/feet. |
| 8. Post-Viral Syndromes (e.g., Long COVID) | Viral infections can trigger a prolonged, dysregulated immune response and cellular energy (mitochondrial) dysfunction. | Shortness of breath, heart palpitations, persistent cough, loss of taste/smell (in COVID), body aches. |
| 9. Heart Disease (e.g., Heart Failure) | A weakened heart can't pump blood efficiently, depriving muscles and organs of the oxygen they need to function. | Shortness of breath (especially when lying down), swelling in legs/ankles, rapid/irregular heartbeat. |
| 10. Adrenal Insufficiency (Addison's Disease) | Adrenal glands don't produce enough cortisol, a hormone essential for energy regulation and stress response. | Salt cravings, low blood pressure, dizziness, darkening of skin (in Addison's), nausea, abdominal pain. |
Look at that table. See how the "other symptoms" vary? That's your clue. A doctor isn't just looking for fatigue; they're trying to see what's holding its hand.
Let me zoom in on one that's often misunderstood: ME/CFS. The fatigue here isn't just being sleepy. It's a pathological depletion. I remember a patient describing it as "having the flu, a hangover, and jet lag all at once, every single day." The Post-Exertional Malaise (PEM) is the true giveaway. You might feel okay during a short walk, but 36 hours later, you're bedbound. This delayed crash is a hallmark most other conditions don't have.
Navigating the Diagnosis Journey: What to Expect
Walking into a doctor's office saying "I'm tired" is a surefire way to get a pat on the back and a suggestion to sleep more. You need to be your own best advocate. Here’s how.
Before the Appointment: Become a Detective
Keep a Fatigue & Symptom Journal for two weeks. This is non-negotiable. Don't just write "tired." Note:
- Timing: Is it worse in the morning or evening?
- Triggers: Does a 20-minute walk wipe you out for two days? (PEM alert).
- Quality: "Heavy limbs," "brain fog," "body aches." Be specific.
- Associated Symptoms: Note any pain, fever, mood changes, digestive issues.
This log turns you from a vague complainer into a provider of crucial clinical data.
During the Appointment: How to Talk to Your Doctor
Lead with your data. "Doctor, I've been experiencing extreme fatigue for [X] weeks/months. It's different from normal tiredness because [use your journal details]. I've also noticed [mention 1-2 other key symptoms, e.g., 'my joints ache' or 'I'm always cold']."
Expect a stepwise diagnostic approach. They'll likely start with common, easily testable causes. According to the National Institutes of Health (NIH), the initial workup often includes:
- Blood Tests: Complete Blood Count (CBC for anemia), Thyroid-Stimulating Hormone (TSH), fasting glucose, iron studies, vitamin D and B12 levels, basic metabolic panel.
- Physical Exam: Checking for swollen lymph nodes, abnormal heart/lung sounds, thyroid enlargement, signs of autoimmune disease like rashes.
If these are normal and fatigue persists, the investigation deepens. This may involve tests for inflammation (ESR, CRP), autoimmune markers (ANA), or a sleep study. The Centers for Disease Control and Prevention (CDC) provides specific diagnostic criteria for conditions like ME/CFS, which is a diagnosis of exclusion.
Red Flags: When Should You Absolutely See a Doctor?
Don't wait. See a doctor immediately if your extreme fatigue is accompanied by any of the following:
Shortness of breath or chest pain. This could indicate a heart or lung problem.
Severe abdominal, pelvic, or back pain. Possible internal issues.
Unexplained, significant weight loss. A classic sign of several serious illnesses.
Blurred vision, confusion, or dizziness to the point of fainting.
Thoughts of harming yourself. Fatigue from depression can be severe and dangerous.
If you don't have these emergency symptoms but your fatigue has lasted more than two weeks and is disrupting your life, schedule an appointment. It's valid. It's necessary.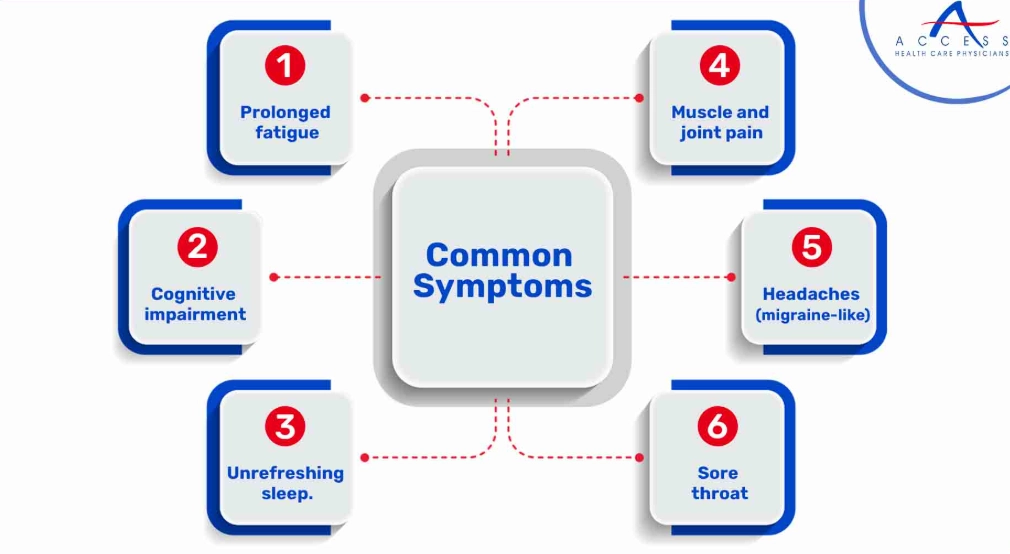
Your Fatigue Questions, Answered
 My fatigue is terrible, but I force myself to exercise hard hoping to "boost my energy." Is this the right approach?
My fatigue is terrible, but I force myself to exercise hard hoping to "boost my energy." Is this the right approach? The takeaway? Extreme fatigue that won't quit is your body sending a high-priority message. It's not a personal failing or a lack of willpower. It's a symptom—and often the first one—of a range of conditions that need and deserve medical attention. By understanding the possibilities, tracking your symptoms precisely, and partnering proactively with your doctor, you can move from simply feeling exhausted to finding a path toward answers and effective management.
The takeaway? Extreme fatigue that won't quit is your body sending a high-priority message. It's not a personal failing or a lack of willpower. It's a symptom—and often the first one—of a range of conditions that need and deserve medical attention. By understanding the possibilities, tracking your symptoms precisely, and partnering proactively with your doctor, you can move from simply feeling exhausted to finding a path toward answers and effective management.
Reader Comments