You toss and turn, watch the clock, and drag yourself out of bed feeling like you never slept. Sound familiar? For years, I just chalked it up to stress, a bad mattress, or too much coffee. It took a partner mentioning my gasping sounds at night and a near-miss at work due to brain fog for me to finally ask the real question: could this be a sleep disorder? The answer was yes—it was sleep apnea. The process of figuring it out was less about a single "aha!" moment and more about connecting a series of dots I'd been ignoring. Let's connect those dots for you.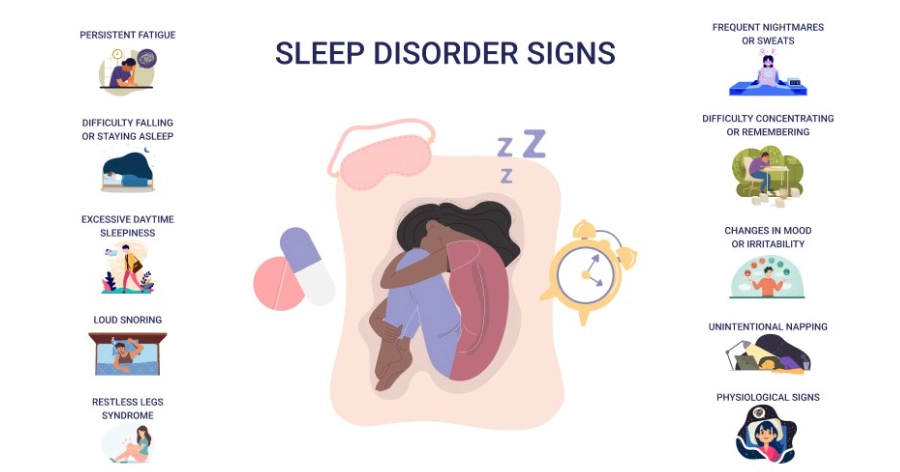
What You'll Find in This Guide
The Red Flags: Common Signs You Might Have a Sleep Disorder
Most people fixate on the night. Did I sleep? How long? But a huge mistake is ignoring what happens during the day. Your daytime function is the ultimate report card for your sleep quality. Here’s where to look.
The Nighttime Clues (The Obvious Stuff)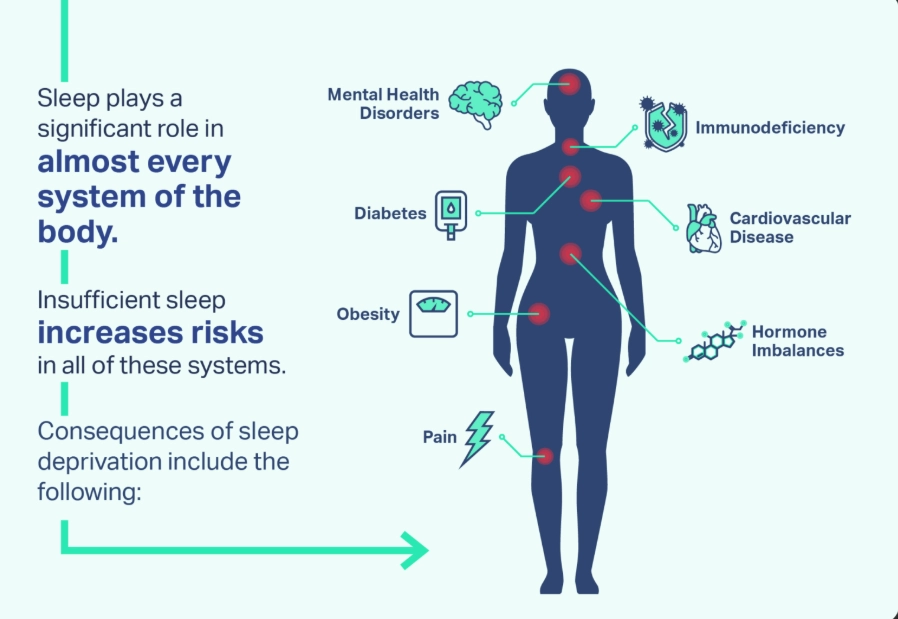
These are the things that might keep you or your partner awake.
- Loud, chronic snoring, especially with pauses or gasps. This isn't just an annoyance; it's a primary sign of obstructive sleep apnea (OSA).
- Taking more than 30 minutes to fall asleep, night after night. Occasional insomnia happens. When it's a pattern, it's a problem.
- Waking up frequently and struggling to get back to sleep. Waking up 2-3 times a night to use the bathroom might be normal for some, but constantly staring at the ceiling isn't.
- Uncomfortable urges to move your legs (Restless Legs Syndrome). That creepy-crawly, gotta-move feeling right as you try to relax is a real neurological signal.
- Acting out dreams—talking, yelling, punching, kicking. This is a potential sign of REM Sleep Behavior Disorder, which is more serious than simple sleep-talking.
The Daytime Symptoms (The Sneaky, Often-Missed Stuff)
This is where people often blame everything else—work, diet, aging. Don't.
Key Insight: Feeling tired is one thing. Experiencing excessive daytime sleepiness (EDS) is another. EDS means you have an overwhelming urge to sleep in situations where you should be alert, like during a meeting, while driving, or in the middle of a conversation. That's a major red flag.
- Waking up exhausted, no matter how long you were in bed. This "non-restorative sleep" is a hallmark.
- Severe morning headaches. Often linked to oxygen dips from sleep apnea.
- Crashing in the afternoon. A 3 PM energy nosedive isn't just a sugar crash.
- Mood changes: irritability, depression, anxiety. Sleep deprivation directly messes with your emotional regulation.
- Brain fog, memory lapses, trouble concentrating. Sleep is when your brain cleans house and files memories. Skip that, and cognition suffers.
- Noticing a drop in your performance at work or school. Mistakes creep in, creativity dries up.

| If You Notice This at Night... | And This During the Day... | It Could Point To... |
|---|---|---|
| Loud snoring, witnessed pauses in breathing | Extreme fatigue, morning headaches, poor concentration | Obstructive Sleep Apnea (OSA) |
| Difficulty falling/staying asleep, waking up too early | Fatigue, irritability, anxiety about sleep itself | Chronic Insomnia Disorder |
| An irresistible urge to move legs, worse at rest | Daytime fatigue from disrupted sleep | Restless Legs Syndrome (RLS) |
| Falling asleep suddenly, at inappropriate times | Cataplexy (sudden muscle weakness), sleep paralysis | Narcolepsy |
Your At-Home Check: How to Perform a Sleep Disorder Self-Assessment
Before you call a doctor, gather evidence. You wouldn't go to a mechanic and just say "car sounds funny." Be your own sleep detective for two weeks.
Step 1: Keep a Detailed Sleep Diary. This is the single most useful tool. Every morning, jot down:
- Time you got into bed / tried to sleep.
- Estimated time it took to fall asleep.
- Number and times of nighttime awakenings.
- Time you woke up for the day.
- Your subjective sleep quality (scale 1-5).
- Any medications, alcohol, or caffeine and their timing.
- How you felt upon waking (refreshed? exhausted?).
Step 2: Use the Epworth Sleepiness Scale (ESS). This is a validated clinical tool you can use at home. Rate your chance of dozing (0=never, 3=high chance) in 8 situations like sitting reading, watching TV, or as a passenger in a car. A score above 10 suggests significant daytime sleepiness worthy of medical attention. You can find the official scale on the Sleep Foundation website.
Step 3: Involve a Bed Partner or Use Technology (Cautiously). Ask your partner: "Do you hear me stop breathing or gasp?" If you sleep alone, a sound recorder app might capture snoring patterns or gasps. Consumer sleep trackers (like Oura, Whoop, or Fitbit) can show restlessness and heart rate spikes, but don't diagnose. They're clues, not conclusions.
A Word of Caution: The internet is full of "quick sleep disorder tests." Avoid any that promise a diagnosis in 5 questions. Self-assessment is about pattern recognition, not self-diagnosis. Its purpose is to give you concrete data to bring to a professional.
How Do Doctors Officially Diagnose a Sleep Disorder?
If your self-check raises concerns, it's time for a professional. This isn't scary; it's systematic. I was nervous about the sleep study, but it was just a night of being monitored to get answers.
Who to See First
Start with your primary care physician (PCP). Bring your sleep diary and ESS score. They can rule out other conditions (thyroid issues, anemia, heart problems) that mimic sleep disorder symptoms. If needed, they'll refer you to a sleep specialist—usually a neurologist, pulmonologist, or psychiatrist with specialized training.
The Gold Standard: The Sleep Study (Polysomnogram)
For disorders like sleep apnea, narcolepsy, or periodic limb movement disorder, this is often necessary. It's not just about "seeing if you sleep."
What it measures, in one night:
- Brain waves (EEG): To stage your sleep (light, deep, REM).
- Eye movements (EOG): To identify REM sleep.
- Muscle activity (EMG): For leg movements and REM behavior disorder.
- Heart rhythm (ECG): To monitor cardiac effects.
- Breathing effort and airflow: To detect apneas (pauses) and hypopneas (shallow breathing).
- Blood oxygen levels: To see if your oxygen drops during events.
You might do this in a lab (a comfortable private room) or, increasingly, with a home sleep apnea test (HSAT)—a simplified device you use in your own bed. An HSAT is great for diagnosing moderate-to-severe OSA but can't diagnose all sleep disorders.
The Diagnosis and the Number That Matters: AHI
For sleep apnea, the key metric is the Apnea-Hypopnea Index (AHI)—the number of breathing pauses per hour of sleep.
- AHI 5-15: Mild sleep apnea.
- AHI 15-30: Moderate sleep apnea.
- AHI >30: Severe sleep apnea.
My AHI was 28. Seeing that number made it real—it wasn't just in my head. It was happening to my body 28 times every hour.
What to Do Next: Your Action Plan After Recognizing the Signs
Okay, you see the signs. Here's what to do, in order.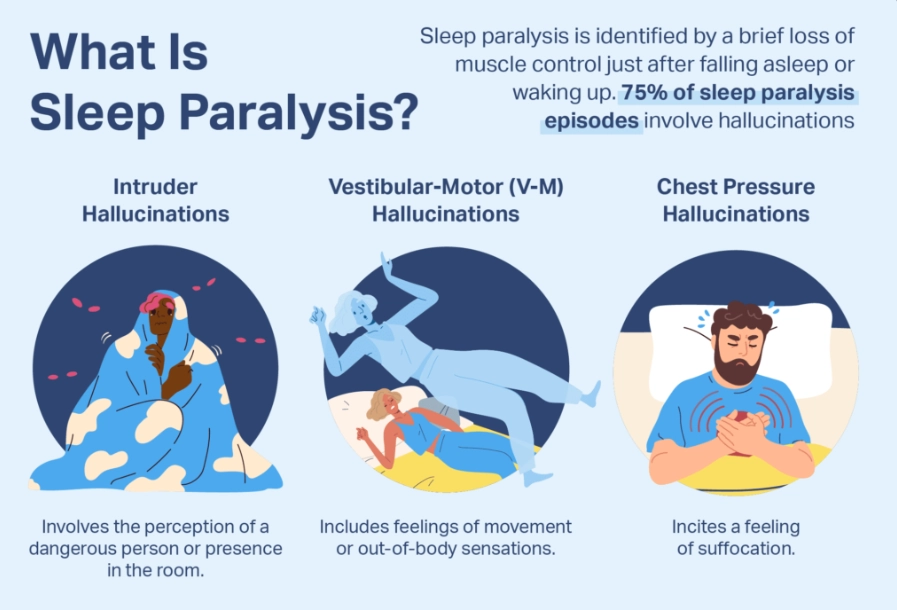
1. Don't Panic, But Don't Delay. Sleep disorders are highly treatable, but letting them fester worsens health risks (hypertension, heart disease, diabetes, depression).
2. Schedule That Doctor's Appointment. Use your sleep diary as your script. Say: "I've been tracking my sleep for two weeks. I'm taking over 45 minutes to fall asleep, my ESS score is 14, and I'm struggling at work. I'm concerned I might have a sleep disorder." This gets you taken seriously.
3. Explore Treatment Options with an Open Mind. Treatment depends on the diagnosis.
- For Sleep Apnea: CPAP therapy is the frontline treatment and is far more comfortable and quiet than it was 10 years ago. Oral appliances or surgery are options for some.
- For Insomnia: The first-line treatment is Cognitive Behavioral Therapy for Insomnia (CBT-I), not sleeping pills. It's a skills-based program that addresses the thoughts and behaviors ruining your sleep. The American Psychological Association has resources on finding a CBT-I provider.
- For RLS: Lifestyle changes, iron supplements (if levels are low), and specific medications can help.
The goal isn't just to sleep more. It's to sleep better and reclaim your days.
Your Questions Answered: Sleep Disorder Diagnosis FAQ
 I'm terrified of a sleep study. What's it really like?
I'm terrified of a sleep study. What's it really like?
Reader Comments