You're staring at the ceiling at 3 AM for the third night in a row. The thought "what helps you sleep medicine" has gone from a passing curiosity to a desperate search. The pharmacy aisle is overwhelming, and you've heard scary stories about prescription sleep pills. Let's cut through the noise. This isn't about pushing pills; it's a clear-eyed guide to the actual tools available, from the melatonin gummy on the shelf to the prescription your doctor might discuss. We'll look at what works, what doesn't, and the crucial safety rules most people gloss over.
What You'll Find in This Guide
Over-the-Counter (OTC) Sleep Aids: The First Stop
Most people start here. It's accessible and feels less serious than seeing a doctor. But "over-the-counter" doesn't mean "no consequences." Understanding the active ingredient is everything.
Melatonin Supplements: The Sleep Hormone
Melatonin is your body's natural "it's dark, time to wind down" signal. Supplements can help reset a confused internal clock. Here's the expert twist most blogs miss: Dose matters less than timing. Taking 10 mg at bedtime when you're already in bed is often useless and can cause morning grogginess. The key is taking a small dose (0.5 mg to 3 mg) 1-2 hours before your desired bedtime. It's a schedule cue, not a knockout punch.
Best for: Jet lag, shift work disorder, delayed sleep phase syndrome (night owls trying to sleep earlier).
Common mistake: Using it as a general sleep aid for anxiety-induced insomnia. It won't quiet a racing mind.
Antihistamines (Diphenhydramine, Doxylamine)
These are the active ingredients in brands like Benadryl (diphenhydramine) and Unisom (doxylamine). They block histamine, a brain chemical involved in wakefulness. They can make you drowsy, but here's the big warning: Your body builds tolerance to the sedative effect incredibly fast, often within 3-4 nights. What doesn't fade as quickly are the anticholinergic side effects—dry mouth, next-day brain fog, constipation, and urinary retention. For older adults, long-term use is linked to a higher risk of dementia.
My advice? Treat these as emergency-use-only, maybe for a night or two before a big presentation when you absolutely must sleep. They are not a long-term solution.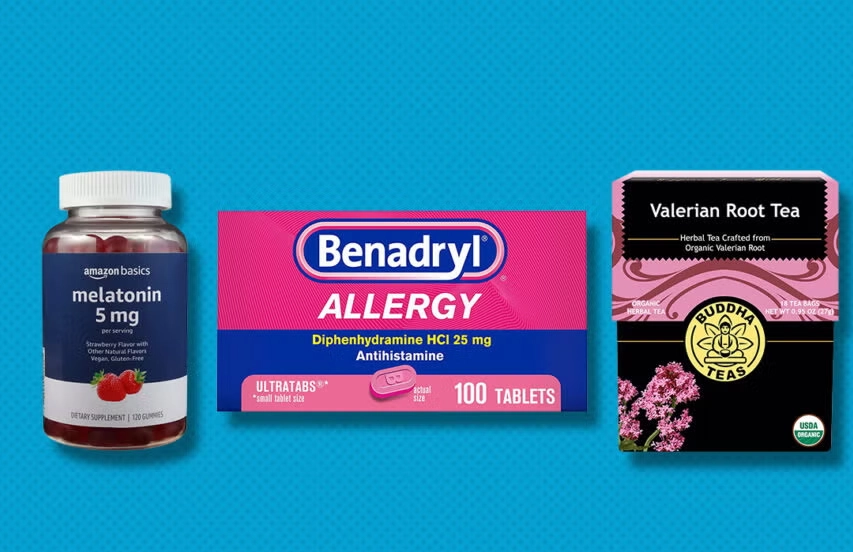
Valerian Root, Chamomile, and Other Herbal Remedies
The evidence here is mixed. Some studies show modest benefits for mild sleep issues. Valerian might help with sleep quality, and chamomile tea's ritual is itself relaxing. The problem is lack of standardization. One bottle's potency can differ wildly from another. If you try them, give it a few weeks and buy from a reputable brand that does third-party testing (look for USP or NSF seals). Don't expect a dramatic, medication-like effect.
| Type | Common Names | How It Might Help | Key Limitation / Risk | Best For... |
|---|---|---|---|---|
| Melatonin | Natrol, Nature's Bounty, various gummies | Resets sleep-wake timing | Ineffective for anxiety; timing is critical | Jet lag, circadian rhythm issues |
| Antihistamine (Diphenhydramine) | Benadryl, ZzzQuil, generic sleep aids | Sedation through histamine blockade | Rapid tolerance, next-day grogginess, anticholinergic risks | Very occasional, short-term use |
| Antihistamine (Doxylamine) | Unisom SleepTabs | Similar sedation, slightly longer-lasting | Same as diphenhydramine; can be very groggy the next day | Very occasional, short-term use |
| Valerian Root | Various supplements and teas | Mild sedative/anxiolytic effect | Weak evidence, variable product quality | Mild sleep anxiety, as part of a wind-down routine |
Prescription Sleep Medications: When OTC Isn't Enough
This is where you need a doctor. These are powerful tools with specific risks and benefits. They are typically prescribed for short-term use (a few weeks) to break the cycle of chronic insomnia, alongside behavioral therapy. Let's demystify the main classes.
"Z-Drugs" (Non-Benzodiazepine Receptor Agonists)
Drugs like zolpidem (Ambien), eszopiclone (Lunesta), and zaleplon (Sonata). They target a specific subset of GABA receptors to promote sleep with (theoretically) less risk of dependence than older drugs.
The reality check: Dependence and tolerance still happen. The most concerning side effect is complex sleep behaviors—sleepwalking, sleep-driving, sleep-eating. I've had patients who woke up to find they'd ordered strange items online with no memory of it. You must take these only when you can dedicate a full 7-8 hours to sleep. The FDA has mandated lower recommended doses for women because they metabolize the drug more slowly.
Benzodiazepines
Drugs like temazepam (Restoril), lorazepam (Ativan), clonazepam (Klonopin). These are older, broader-acting sedatives. They are effective but come with a high risk of tolerance (needing more for the same effect), dependence, and withdrawal. They also impair memory and balance. Frankly, they are poor first-line choices for primary insomnia today. They are sometimes used for sleep anxiety, but even then, only very short-term.
DORA Drugs (Dual Orexin Receptor Antagonists)
The newer class, including suvorexant (Belsomra) and lemborexant (Dayvigo). These work differently by blocking orexin, a brain chemical that promotes wakefulness. Think of it as turning down the "wakefulness" signal instead of cranking up the "sleepiness" signal. Side effects can include next-day drowsiness, but they may have a lower risk of dependence and abnormal sleep behaviors. They're a more targeted option, but they're expensive and not always covered by insurance.
Low-Dose Antidepressants
Medications like trazodone, doxepin (Silenor), and mirtazapine are often prescribed "off-label" for sleep at very low doses. They're not addictive, which is a huge plus. Trazodone is probably the most commonly prescribed sleep aid in the US for this reason. Effectiveness varies. Doxepin is interesting—at the tiny 3-6 mg dose for sleep, it's a potent histamine blocker without the rapid tolerance of OTC antihistamines.
Choosing among these isn't a DIY project. A good sleep doctor will consider your specific insomnia type (trouble falling asleep vs. staying asleep), your medical history, other medications, and risk for dependence.
The Non-Negotiable Rules for Using Sleep Medicine Safely
This is where I see the most mistakes, even from people with the best intentions.
- Never Mix with Alcohol. This isn't just a suggestion; it's dangerous. It can lead to severe respiratory depression, memory blackouts, and dangerous behavior.
- Use the Lowest Effective Dose for the Shortest Duration. The goal is to use medication as a temporary bridge while you implement better sleep habits (see below).
- Schedule a Full Sleep Window. If you take a sleep aid at midnight but your alarm goes off at 6 AM, you're setting yourself up for dangerous grogginess.
- Be Brutally Honest with Your Doctor. Tell them about all supplements and OTC drugs you use. That includes the "natural" valerian or the Benadryl you took last week.
- Plan the Exit Strategy Before You Start. Ask your doctor: "What's the plan for tapering off this medication?" If they don't have one, that's a red flag.
What to Do When Sleep Medicine Isn't the Answer (Or the Only Answer)
Pills don't teach skills. For chronic insomnia, medication alone is like using a painkiller for a broken leg without setting the bone. The gold-standard, long-term solution is Cognitive Behavioral Therapy for Insomnia (CBT-I). It's a structured program that addresses the thoughts and behaviors that perpetuate poor sleep. Studies consistently show it's as effective as medication in the short term and more effective in the long term.
You can find certified CBT-I therapists through organizations like the American Psychological Association or use digital programs like Sleepio or CBT-I Coach. Many people benefit from a combination: short-term medication to get some relief, paired with CBT-I to build lasting skills.
Also, don't underestimate the basics that everyone ignores because they sound too simple:
Light: Get bright light first thing in the morning. Dim lights and avoid screens 1-2 hours before bed.
Schedule: Wake up at the same time every day, even weekends. This is more important than a fixed bedtime.
Bed = Sleep (and Sex): If you're awake and frustrated in bed for more than 20 minutes, get up. Go read a boring book in dim light. Only return to bed when sleepy. This breaks the association between bed and anxiety.
Your Top Questions on Sleep Medicine, Answered
Finding what helps you sleep medicine-wise is a process of careful trial, honest communication with a healthcare provider, and pairing any chemical aid with behavioral change. Start with the lowest-impact option that matches your specific problem, respect the safety rules, and always have an eye on building your own ability to sleep without help. That's the real goal.
Reader Comments